
COVID-tivity: Unexpected Inspiration from a Killer Virus
A SILENT DRAMA UNFOLDS IN THE SIM LAB.
 [Listen. Confer. Watch.]
[Listen. Confer. Watch.]
Michael Simpson—a 6’2,” 76-year-old with mild arthritis, a penicillin allergy, and type 2 diabetes—stops talking, moans, lays still, and quietly begins his descent into septic shock.
Despite having received intravenous fluids, his vital signs run haywire: his heart rate spikes, and his blood pressure tanks. Simpson’s lactate and white blood cell count scream potential sepsis. His groans are replaced by quiet, then tinny chatter from a small group of fourth-year nursing students discussing what to do next as they peer at Simpson in his hospital bed over the internet platform Zoom, his nurse at the bedside, waiting for their instructions.
On this day, that bedside nurse is being role-played by instructor Rachel Bankhead, who’s live in the Clinical Simulation Learning Center on the third floor of McLeod Hall dozens, or even hundreds of miles away from her students who’ve tuned into class. With masked cameraman Matthew Adamski, CSLC simulation specialist, filming on an iPad, students guide Bankhead’s administration of fluids and ceftriaxone, painstakingly instruct her about how to begin an IV infusion of Levophed, and titrate the dose until he stabilizes. It isn’t long before Simpson, a high-fidelity mannequin manipulated by Ryne Ackard, CSLC director, from the nearby control room, comes to, and moans again.
Then little things start to go wrong.
There’s a crimp in the IV line; students help Bankhead reestablish its flow. An alarm on the Alaris pump beeps; they tell her what it means, and how to clear it. She asks a question about Simpson’s lactate levels; they explain its significance in septic patients. Thrust into the role of preceptors, Bankhead’s students think critically, reason clinically, and plot a path forward for care.
“If they can teach me, playing the role of a new nurse,” observed Bankhead of the “flipped” virtual simulation she created in which students instruct and faculty facilitate, “they can definitely also be confident in their own ability, too.”
 WELCOME TO THE WORLD OF NURSING EDUCATION AMID COVID-19, a full-throttle effort to transmit rich, relevant, experiential learning into virtual classrooms. When the pandemic shuttered UVA in late March, faculty and staff quickly pivoted learning online, in the process dreaming up new approaches to their work.
WELCOME TO THE WORLD OF NURSING EDUCATION AMID COVID-19, a full-throttle effort to transmit rich, relevant, experiential learning into virtual classrooms. When the pandemic shuttered UVA in late March, faculty and staff quickly pivoted learning online, in the process dreaming up new approaches to their work.
Some completely overhauled existing learning methods, like assistant professor Sarah Craig, who developed novel virtual NCLEX practice tests to ready students for their boards, and clinical instructor Donna Bindig, who used a combination of simulation software, associated readings, and live discussion and demonstrations to strengthen their clinical skills.
- [more: Sarah Craig on TAKING TEST PREP VIRTUAL]
- [more: Elizabeth Taliaferro-Jones on PRACTICUM, PROFESSIONALISM, and the COVID PAUSE]
- [more: Donna Bindig on LEARNING AS SCAFFOLDING]
Clinical instructor Elizabeth Taliaferro-Jones assigned imaginative writing assignments using COVID scenarios to test students’ clinical mettle, sparking animated discussions she called “some of the best of [her] career.”
“Even though I missed having them at the hospital, I was able to see their beautiful faces each week, and lighten their load, comforting them—trying to, anyway—and being an active listener.
"Really, I was using the same techniques I always do,” explained Bindig, “but it was in a virtual setting.”
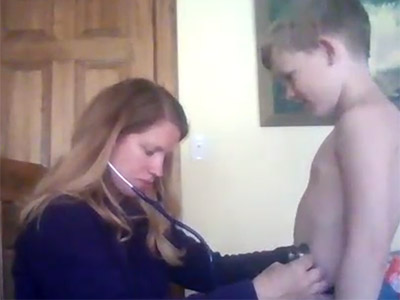 Others taught skills live—assessing heart and bowel sounds, conducting neurological and hearing tests, even doing eye, ear, throat, and nose exams—using loved ones as patients, like assistant professor Beth Hundt (PhD `18), and clinical instructors Ginger Richardson (at right, with her young son as her pediatric patient) and Katie Morgan (above, demonstrating clinical assessment skills using her husband) whose students received assessment kits by mail, with otoscopes, tongue depressors, reflex hammers, even tuning forks.
Others taught skills live—assessing heart and bowel sounds, conducting neurological and hearing tests, even doing eye, ear, throat, and nose exams—using loved ones as patients, like assistant professor Beth Hundt (PhD `18), and clinical instructors Ginger Richardson (at right, with her young son as her pediatric patient) and Katie Morgan (above, demonstrating clinical assessment skills using her husband) whose students received assessment kits by mail, with otoscopes, tongue depressors, reflex hammers, even tuning forks.
“It takes a village,” said Hundt, whose husband, Keith Crews, a UVA Health respiratory therapist, has repeatedly played her patient this summer, “this year more than ever.”
COVID-tivity: Lizze Lawwill, nurse practitioner + hospitalist
Others determined to make their virtual work a simulacrum for their connectivity pre-pandemic. Through spring and summer, BSN program manager Lynn Coyner has remained doggedly available tending disappointed students, monitoring classroom and clinical progress, supporting faculty adjusting to online learning, and even welcoming small groups of new students with virtual orientations and “get to know you games.”
- [more: Lynn Coyner on A PERPETUALLY-OPEN DOOR]
Assistant professor Amy Boitnott (DNP `08, at left, with instructor Ginger Richarson at a virtual celebration of NP students) kept her classes entirely synchronous (though lectures are still available for students in the Cloud), drawing near perfect attendance despite a “little technical awkwardness.” Boitnott, who “feeds off students’ energy in class,” managed to maintain much of the back and forth of her in-person classes, including her signature gratitude check-ins, lively discussions, and ample space and opportunity for students to “rush the podium” to talk after class.
“I knew I had to be the very best I could be,” said Boitnott, who’s teaching both advanced practice nurses and CNL students this summer. “I told them, ‘It’s going to be messy, but together, we’re going to continue to learn.’ And people really showed up.”
- [more: Amy Boitnott ON GRACE, MERCY, and ZOOM]
Even history lessons, like those learned in the ethics class taught by professors Beth Epstein (BSN `94, PhD `07) and Mary Faith Marshall, who scrapped their syllabus mid-March to pivot to pandemic science and the ethical dilemmas therein (the result of what Epstein called an “ah-ha” moment in the middle of the night)—proved “immediately relevant.”
“It was incredible,” said Lizze Lawwill (BSN `05, DNP `20), a hospitalist at Sentara Martha Jefferson Hospital’s respiratory unit, who took the course, and is a clinical instructor at the School, too. “We looked at SARS, influenza, H1N1 in 2009, and how you make decisions if resources become scarce.”
If some uncertainty remains as in-person classes begin again August 25, educators, learners, and practitioners are settling into living, learning, and practicing amid COVID. That they’re gleaning wisdom about COVID is a given. But more than simply coping, they’re drawing strength and new ideas from it, too.
And while students, faculty, staff, and clinicians still feel anxiety over the murky challenges posed by the pandemic—for Lawwill, that’s balancing how and when to hospitalize which patients, given transmission risks, and preventing the virus’s spread to colleagues and her family—other things have become crystal clear.
“I get to wear a mask,” Lawwill’s three-year old daughter Madeline observed, as her mother tied a bright yellow mask over her face before the two entered the grocery store last month, “and be a superhero like you.”
[Qualify.* Intervene. Respond.]
Last spring, COVID brought many research projects to a screeching halt, given stay-at-home orders, physical distancing requirements, and guidelines governing human contact. And since the mid-June ramp back up, it’s created layers of additional considerations: PPE protocols, recruitment and data collection changes, the need to reconfigure global projects, and frustrating delays in grant approvals, journal submissions, peer reviews, and publications.
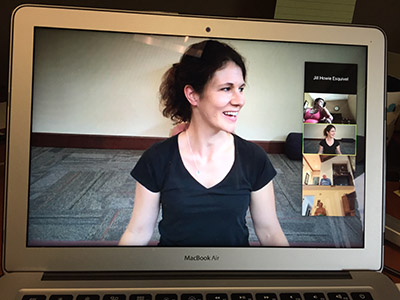 But for some, like associate professor Jill Howie-Esquivel, COVID actually strengthened the relevance of projects already underway
But for some, like associate professor Jill Howie-Esquivel, COVID actually strengthened the relevance of projects already underway
[At left, exercise physiologist Shannon Wells leads a group of patients with heart failure through the gentle, live, virtual exercise pilot program developed by associate professor Jill Howie-Esquivel].
Late last winter, in the live, virtual exercise class she’d developed for rural heart failure patients, Howie-Esquivel had already observed participants dropping in ten, 15, even 25 minutes early on Zoom. They’d chat, set up their yoga mats and adjust their iPads, and gently joke with and chide one another.
“How’d you get heart failure?” one male participant asked another.
“Oh, my mother gave it to me,” another chortled back.
When COVID struck, the pattern grew more pronounced. Participants told Howie-Esquivel the class made them feel less isolated. These strangers had become a community. And everyone consistently came.
“In research, you’re excited if somebody does something 75 percent of the time,” laughed Howie-Esquivel, whose study continues through 2021. “Participants never do something 100 percent of the time, and yet these people did.”
COVID’s made others widen their scholarly scope, too. Since quarantine, maternal mental health scholar Jeanne Alhusen, associate dean for research, has broadened her study of women living with disabilities to understand how the virus “magnified existing isolation impacting their mental health,” affecting their access to reproductive and family planning care.  Associate professor Pamela DeGuzman (BSN `96, MSN `00, PhD `12) expanded her pilot study of a nurse-led intervention for cancer survivors to include those who battled lung as well as head and neck cancers, with the aim of addressing rural patients’ psycho-social wellbeing by, among other things, measuring distress. Still others, like assistant professor Meghan Mattos (MSN `09), are currently working to qualify* older adults’ loneliness through interviews, with the aim of developing and nimbly delivering interventions to prevent the cascade of ill health effects isolation can bring.
Associate professor Pamela DeGuzman (BSN `96, MSN `00, PhD `12) expanded her pilot study of a nurse-led intervention for cancer survivors to include those who battled lung as well as head and neck cancers, with the aim of addressing rural patients’ psycho-social wellbeing by, among other things, measuring distress. Still others, like assistant professor Meghan Mattos (MSN `09), are currently working to qualify* older adults’ loneliness through interviews, with the aim of developing and nimbly delivering interventions to prevent the cascade of ill health effects isolation can bring.
- [more: Pam DeGuzman on WHAT RURAL CANCER SURVIVORS NEED]
It’s a powerful reminder, said Alhusen, that an intervention’s how is just as important as its what.
“There are opportunities here to deliver treatments and interventions in ways we previously haven’t thought of,” said Alhusen, “and we’re looking to the virtual world to get patients and families and communities what they need.”
“There may be a lot of research dollars going toward COVID,” she added, “but it’s not all about cures, vaccines, or antibody testing. Funders are starting to recognize the social impact it’s having, and our faculty are well-poised to respond.”
*Qualitative research is a research method that seeks to explore and understand personal experiences.
[Hear. Remember. See.]
COVID’s powerful lessons—concurrent with a national discussion of racial injustice, civil rights, and violence in American policing—have also stirred poignant learning about inequality, racial justice, and, in many deepened long-brewing activism.
In the days after George Floyd’s murder, many students, faculty, staff, and clinicians gathered for online discussions together, attended demonstrations, used social media as a platform to share stories, and attended events like the June 5 White Coast for Black Lives gathering, which drew hundreds to “take a knee” at the Memorial for Enslaved Laborers near the Rotunda.
 In Richmond, Emily Cramer (BSN `15) and Amy Newcombe (CNL `15), both VCU Medical Center nurses, quickly resolved to offer emergency first aid when they saw peaceful protesters teargassed in a Black Lives Matter march.
In Richmond, Emily Cramer (BSN `15) and Amy Newcombe (CNL `15), both VCU Medical Center nurses, quickly resolved to offer emergency first aid when they saw peaceful protesters teargassed in a Black Lives Matter march.
“It’s one small way I can help,” said Cramer, who carried a sign that said, FIRST AID AND WATER (at right, photo by Amy Newcombe, CNL `15). “A lot of people are really proud to be nurses right now, so to them I say, ‘Put those words into action, and help people when they need it.’”
In other cases, when the quarantine curtailed the ability to offer care in person, it concurrently strengthened the resolve to advocate. That was true for Katie Bullard (BSN `20), who watched from her Charlottesville apartment as her 56-year-old father John battled coronavirus in her parents’ Long Island, NY, home. At the same time, Bullard—who’d worked at a small group home for cognitively and physically disabled adults back in Medford, NY—received word that her clients, who ranged in age from 47 to 76, began to contract COVID.
The first to die was a man in his 70s. Soon after, three more residents contracted the virus, were hospitalized, and died. By early May, as Bullard’s father recovered, five of the group home’s eight residents were dead, including the two with whom Bullard worked most closely.
When she thinks about it now, Bullard (below, in the foreground, with a fellow member of the BSN class of 2020) feels a swell of anger that this population—that continued to attend day programs days after schools and universities shut down—wasn’t better protected. That they died alone in the hospital, their caregivers—their only family, in many cases—prohibited from being at their side. That policies weren’t put in place to assure their well-being. And that their deaths—like their lives—were largely invisible to the outside world. Since the tragedy, Bullard resolved to become an even stronger advocate for people living with disabilities.
Some of that work means showing up. Though the COVID crisis has abated in New York, it was July 2 before Bullard, fellow staff, and the remaining residents could memorialize their dead. The service paid tribute to the five who’d died, including a woman in her 60s whom Bullard had cared for closely: chatting as she helped her shower, nodding as she talked, and smiling wordlessly as Bullard painted her fingernails.
 Heard. Remembered. Seen.
Heard. Remembered. Seen.
“UVA has prepared us well,” said Bullard, who’s spending this summer at her parents’ home studying for the NCLEX, “but all this has shaped me, and gotten me ready for my career as a nurse—even though I’ve been … we’ve been, over quite a few bumps."
[Invent. Adjust. Build.]
In the shade of her Richmond home, DNP student and emergency room nurse Ashley Apple (BSN `18, MSN `20) muses that the backyard oasis she created during the pandemic—with its expansive gardens and new chicken coop—helped her “operationalize [her] COVID anxiety.”
COVID-tivity: Ashley Apple, ER nurse + DNP student
“Not really knowing what to expect, and what comes next, can be really disconcerting,” said Apple, who works in emergency rooms across Bon Secours Mercy Health's many sites in and around Richmond, “so taking on a project like this that takes a lot of work, drive, and focus was a good way to channel that nervous energy into something that was really positive and meaningful.”
The project took six weeks and gave Apple, her wife, Aisha, and children Gavin, 8, and Stella, 6, something positive to focus on during a time when worry and isolation proved vexing.
These days, as Apple writes her capstone proposal, she gazes through the window of her home office at the garden teeming with corn (Gavin’s idea), squash, cucumbers, and watermelon (Stella’s project). From that vantage, she can just glimpse the coop where the family's flock of chickens murmur, gurgle, and peck at the ground.
The whole process was actually a lot like nursing itself, mused Apple.
“I had to be creative,” she said, “tackle tough problems that you don’t know how to fix, but you do, and work with what you have.
"Circumstances change," added Apple. "You have to be adaptable.”

